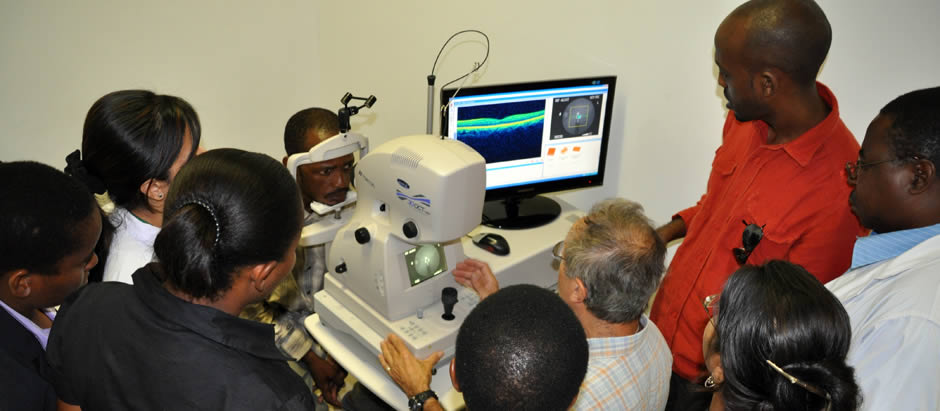
Building networks to combat preventable blindness across the Commonwealth
The Consortium is addressing the growing burden of eye disease across the Commonwealth by continuing to develop three networks. These networks are enabling Commonwealth eye health professionals to share their experiences and knowledge in diabetic retinopathy, retinoblastoma and retinopathy of prematurity. Two of these networks function as part of the VISION 2020 LINKS Programme, the DR-NET and RB-NET, and are a network of hospital-based training LINKS between overseas and UK partners.
Throughout the three networks, partner hospitals in Africa, Asia, the Pacific and the Caribbean will develop appropriate strategies and services to screen patients.
By catching these diseases early, more people will have their sight saved and the number of people going blind unnecessarily across the Commonwealth will be reduced