By Christian Suharlim (Harvard T.H. Chan School of Public Health)
Cross-posted at immunizationeconomics.org.
Imagine you own a parking garage business. Half of your costs are associated with owning, building, and maintaining the property – a third for labor costs associated with managing the operations – and the rest for promotional materials, security, and insurance. Businesses often maintain detailed information on the cost structure of their operations. They use this information to help them better allocate resources, identify more efficient ways of operating, and ultimately free up funds for business expansion or profit.
However, the use of such methods to analyze public health services is less common.
In a new study published in Health Policy and Planning, a research team from the Harvard T.H. Chan School of Public Health examined the cost structure of routine immunization programs in six countries. These were Benin, Ghana, Honduras, Moldova, Uganda and Zambia.
They found that 77-93% of the total cost of immunization program was attributable to the healthcare facility. The remaining costs were primarily associated with logistical and administrative costs at the national and subnational health offices. Further unpacking the facility-level costs, they found that 63% of these costs were associated with immunization delivery via facility-based service or outreach service, with the remaining 37% spent on supply chain, program management, social mobilization, monitoring and evaluation.
Lead author Fangli Geng shared major takeaways from the findings. “We found that labor costs were a key driver of the facility-level delivery costs. When we compare more and less efficient sites, we find that labor costs explain a lot of this difference. At the moment, we’re exploring to what extent these costs are explained by contextual factors such as geographical barriers or improved quality,” she said.
“Management and administrative activities account for about a third of facility-level delivery costs.” Geng continued. “Innovations that make these activities more efficient could free up substantial resources to provide better services for underserved populations, such as those in geographically remote areas and the socially marginalized.”
This study comes at a time where novel methods are being piloted in the field of immunization delivery. In October of last year, Gavi partnered with UPS and Zipline to use drone technology to deliver blood supplies to health clinics in Rwanda. This drone-assisted blood supplies delivery serve as a test for other health purposes, including vaccine delivery. Similarly, pilot projects utilizing mobile phones (M-Health) such as text reminders for immunization programs have been well received in low-and-middle income county settings. These novel approaches will add to the toolbox for improving social mobilization.
Geng’s research is part of a larger project called EPIC – Expanded Program on Immunization Costing, Financing, and Efficiency, led by the Harvard T.H. Chan School of Public Health.
“One major goal for EPIC is to figure out how to routinely collect cost data – so that immunization managers can perform these kinds of cost structure analysis real-time and make optimal resource allocation decisions,” noted Stephen Resch, principal investigator of the EPIC project and the deputy director of Harvard’s Center for Health Decision Science.
This research adds to the understanding of the detailed cost structure and site-efficiency of routine immunization programs, further understanding of the site-level characteristics could reveal approaches to improve efficiency and performance of immunization delivery sites. Comprehensive resources for researchers and policy makers associated with this research and the EPIC project are available on their website, immunizationeconomics.org.
“The cost structure of routine infant immunization services: a systematic analysis of six countries,” Fangli Geng, Christian Suharlim, Logan Brenzel, Stephen C Resch, and Nicolas A Menzies, Health Policy and Planning, online May 31, 2017, doi: 10.1093/heapol/czx067
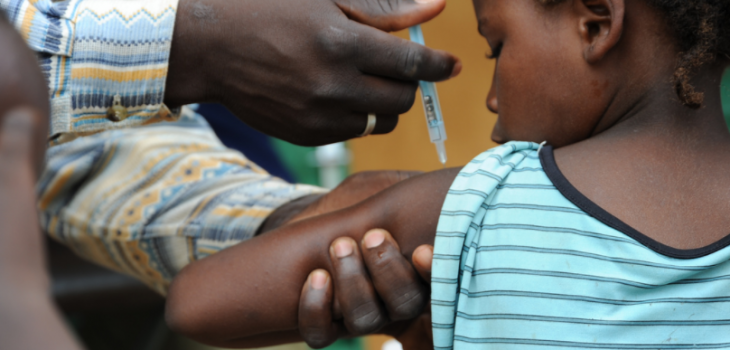
Image credit: PATH Global Health